Dr. Angelique Campen is an ER doctor at Providence Saint Joseph Emergency Department, a Clinical Instructor of Emergency Medicine at UCLA Medical Center, and the CMO and Founder of Vital Medical Services. Follow her down to earth evidence based information at @glamERdoc.
1) Amazingly we are now in our 9th month dealing with the coronavirus. Recent reports indicate another surge in positive cases, both locally and nationally. Is that reflected in the traffic you are currently seeing in the ER?
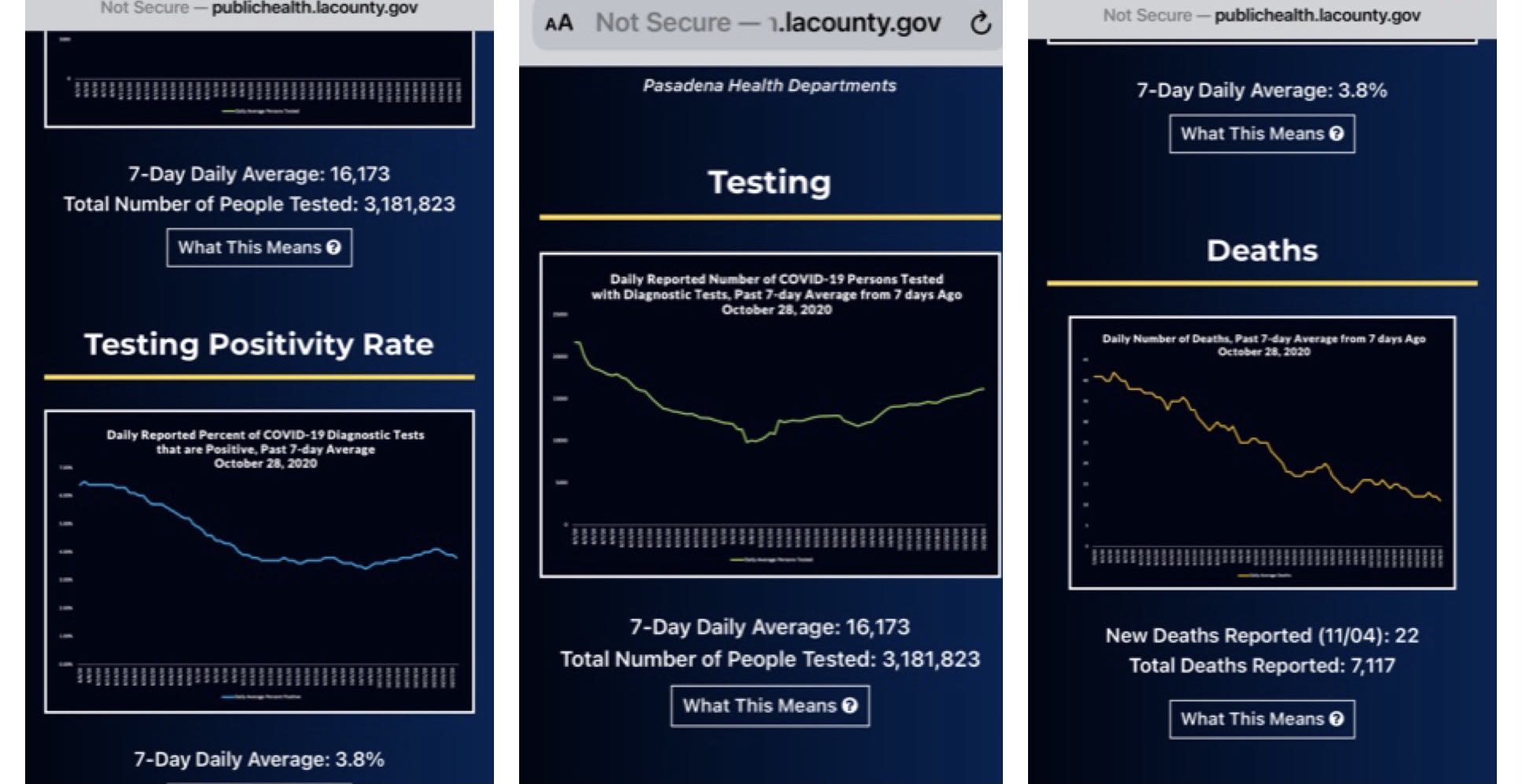
I do detect an increase in positive cases. The increase in numbers however is also in the face of increasing testing capabilities and increase in access to testing. Mortality rates are still decreasing and percentage of tests positive is holding steady in Los Angeles at 3.5%.
2) How different is treating a coronavirus case today compared to early in the pandemic?
With experience we obviously have a better handle on how to treat the infection. We still do not have many choices for medications, but it is clear that steroids (decahedron) and convalescent plasma (donated by previously infected people) helps those with severe illness. Like the flu, covid-19 in healthy people doesn’t have any treatment and just requires supportive care: rest, fluids, vitamin C, and time.
3) Are you seeing any trends right now in what groups tend to get coronavirus and also if there are trends in people who don’t tend to get too sick, vs those that do?
There are definitely trends that follow ethnicities. Hispanic, Native American, and black populations tend to get sicker. This goes across socioeconomic levels as well as access to care. My theory is there is something physiologically (such as the expression of the ACE receptor) that differs in different ethnicities that plays a role. Additionally, I find that people with certain risk factors, obesity especially, tend to get much sicker, faster.
4) Now that we are nearly a year into dealing with the virus, what advice do you have for people as we head toward the holidays, to celebrate and spend time with family and friends, but not do so recklessly.
It is clear how to keep yourself safe: clean hands, don’t touch your nose or eyes, and avoid anyone outside of your “bubble” that isn’t wearing a mask. If you plan to gather as a family in a small group that doesn’t live together, it is imperative to get tested prior. Some people carry the virus without any symptoms and can spread it to others.
5) As we head into the new year, what do you think needs to or should happen for there to be a significant reopening of businesses, schools, churches, etc.
I think we know enough about the transmission of the disease to be able to use our health precautions and get back to life. By wearing masks, limiting people in one space, and using screening tests, we should be able to get back to work, school, and fun.
6) Are there any groups of people you think should be tested more frequently (aside from front line workers)?
I think everyone should get tested now together with an antibody test (which tells you if you have had the infection in the last 4-5 months) and then continue to get tested monthly. Because we cannot predict who will be infected and not have symptoms, it’s important to continue to screen the general population. Tests are a simple five second swab in the nose (not a “brain biopsy'; just a weird sensation) that goes to a lab and is analyzed for the RNA of the virus. Results are typically available the next day and insurance typically reimburses the cost. There are also rapid tests available that give a bit less accurate but faster results. It may not detect every positive case, but if a result is positive then we know that an infection is real (it has false negatives but not false positives)
Through Vital Medical Services, I offer both concierge and large scale testing services. 323-788-3409 or vitalmedicalservices.
You can also follow Dr. Campen @glamERdoc.